A report series on lessons learned from PEPFAR's success
Introduction
Reducing HIV infections is one of the targets of the United Nations’ third sustainable development goal to ensure healthy lives and promote well-being for all at all ages. Progress toward this goal and eliminating HIV/AIDS as a public health threat require a deep analysis of data from both program sites and community surveys to illuminate gaps and populations that have been underserved or excluded from care. In particular, data are essential to addressing the unique risks of, and improving the accessibility of services for, women and girls and other key populations, including people who inject drugs (PWID), men who have sex with men (MSM), prisoners, sex workers, and transgender people.
“This Nation can lead the world in sparing innocent people from a plague of nature. ”
— President George W. Bush, State of the Union Address, January 29, 2003
Over the last 20 years, PEPFAR has established a proven track record of employing data to highlight and eliminate clear barriers to care and shape community-informed, community-led approaches to ensure everyone has equitable access. In doing so, PEPFAR has collaborated with private-sector companies, multilateral organizations, and foundations, to develop public-private partnerships (PPPs) to expand the reach of PEPFAR’s programs.
This report series examines the lessons offered by PEPFAR over the last two decades. The first paper in this series discusses the critical importance of data and measurement to developing, managing, and improving programs. The second paper outlines the importance of collaboration, respect, and data-sharing between funders, multilateral organizations, and implementers to ensure every dollar achieves the best results, to eliminate duplication, and to align resources and policies in service to others. The third paper explores the importance of granular, geolocated information to match funding with on-the-ground reality and create a pathway to data-driven and verified equity.
This paper articulates PEPFAR’s use of age-segmented and sex-disaggregated data to define programmatic gaps and pivot to address them head on. It discusses how innovation from peer leads and local implementers, along with the continuous collection and use of data, are the hallmarks of PEPFAR’s successful partnerships for the most vulnerable. In particular, the paper shines a spotlight on the DREAMS (Determined, Resilient, Empowered, AIDS-free, Mentored, and Safe) initiative and Pink Ribbon Red Ribbon (PRRR), which evolved into Go Further.
Download the report (PDF)
View the recommendations
Finding the Missing
From the beginning, President George W. Bush committed that PEPFAR would reach the least fortunate and the most vulnerable. As the president declared in a proclamation to mark World AIDS Day in December 2003, “Fighting HIV/AIDS is not only a great challenge but also a moral imperative for those who believe in the value and dignity of every human life.”
In its first decade, PEPFAR and its partners carried out the largest initiative dedicated to fighting a single disease in history. The program was treating more than 6 million people with lifesaving antiretrovirals (ARVs) and had just celebrated the birth of the 1 millionth baby born HIV-free because of its support at the time of PEPFAR’s 10th annual report to Congress. In 13 countries, PEPFAR and the Global Fund to Fight AIDS, Tuberculosis, and Malaria worked together with national governments and community groups to lower the number of annual new adult HIV infections to below the increase in adults on ARVs each year.
Despite this tremendous progress, the goal to end AIDS required PEPFAR and its partners to dig deeper and understand the transmission, prevention, and treatment of HIV in a more granular manner. One of the challenges in ending AIDS is determining who does not have access to essential prevention or treatment services. Programmatic data show clearly who is receiving care, but do not reveal who is left behind.
Many early efforts to fight the transmission of HIV only reached people who came to clinics seeking care. The wide net PEPFAR cast did not reach many children under 14; diagnosed fewer men than women; missed many young adults, particularly adolescent girls and young women; and overlooked members of key populations. It took years and the implementation of sophisticated data-collection systems and targeted programming to begin to close those gaps.
Beginning in 2004, PEPFAR used modeled estimates from UNAIDS and combined them with extrapolations from the limited data generated by programs on the ground to identify large groups that needed lifesaving treatment. Based on the modeled data and reports from partners, PEPFAR saw that the overwhelming majority of HIV-positive children under age 14 were not receiving treatment. The guidance issued by the Office of the Global AIDS Coordinator, which oversees PEPFAR, for the development of the program’s Country Operational Plans (COPs) for 2006 therefore made scaling up pediatric treatment “an urgent priority.” The program immediately devoted significant resources to the problem. The expectation was that 15% of the clients placed and sustained on ARVs in each PEPFAR country should be children.
Over the next few years, PEPFAR succeeded in placing tens of thousands of children living with HIV on safe and effective treatment. By 2008, PEPFAR was treating 85,900 children, according to its annual report to Congress, up from only 4,800 four years earlier. It recorded 258,000 by 2011.
Nevertheless, qualitative data made clear that a lack of easy-to-use medications remained a major barrier to expanding access to therapy for children even further. Parents had to break up pills for older children and, more problematically, dilute products into liquids to give to younger children by syringes, a complex process. Many of the medications had a bitter taste, and children often would spit them out. In 2006, PEPFAR launched a public-private-partnership with key manufacturers of ARVs, the U.S. Food and Drug Administration (FDA), and members of the community to explore rapid pathways to develop child-friendly products, which have included sprinkles that parents and caregivers can add to porridge and liquid medications that taste better.
But data over the next few years continued to show that many children who needed treatment in PEPFAR countries were not receiving it, and meeting the 15% target remained elusive. In response, the Office of the Global AIDS Coordinator began a program in 2014 called Accelerating Children’s Treatment (ACT), which created targets for each PEPFAR country with a deficit in treatment services for children across all age bands. PEPFAR’s teams in the field and at headquarters charted progress quarterly so the program could evolve in real time and improve implementation site by site, community by community, and quarter by quarter. After the first quarterly reporting period, ACT had been proven immediately successful in achieving the goals for each country and became a model for targeted PPPs.
PEPFAR’s focus on finding better, more palatable medication for children and increasing access to them has continued. This public-private collaboration has resulted in 75 FDA-approved new pediatric formulations entering the market over the past decade, as shown on the agency’s website. In late 2020, the FDA cleared a children’s version of dolutegravir (DTG), the preferred first-line ARV, in a record five months after approving the adult drug. Negotiations with manufacturers have lowered the yearly price of the strawberry-flavored dissolvable tablet in low- and lower-middle-income countries to under $40 per child.
But reaching children was only the beginning when it came to addressing gaps in access to prevention and treatment services. PEPFAR and its partners realized that stubborn chains of adult transmission were occurring even as national data showed remarkable progress. It became essential to understand who in each community was not being reached as the governments of the countries in which PEPFAR invests committed to reaching the “90/90/90” goals by 2020 and “95-95-95” by 2030 (at least 95% of all people should know their HIV status; at least 95% of all people with diagnosed HIV should receive antiretroviral [ARV] treatment and continue it; and at least 95% of all people on ARV therapy should have undetectable levels of the virus in their blood). After 10 years of implementation, PEPFAR and its partners knew who they were seeing in their clinics and hospitals, but still did not have a good idea of how many people had never been tested, did not know their status, and thus were not seeking out prevention or treatment.
To determine who implementers were missing, PEPFAR funded countrywide community surveys designed to define each of these parameters (95, 95, 95) by five-year age bands. The Office of the Global AIDS Coordinator planned the first of these Population-Based HIV Impact surveys (PHIAs) in 2014 and 2015 with the Centers for Disease Control and Prevention and ICAP at Columbia University. Implementation began at the end of 2015 in all countries with a generalized HIV epidemic (defined as one in which most new infections are from heterosexual contact in the general population and the overall nationwide percentage of adults infected is over 2%) and an annual PEPFAR investment of over $25 million. For the first time, PEPFAR would have comprehensive, community-level data on who was receiving services as well as measured HIV prevalence (overall percentage of adults infected) and incidence (annual rate of new infections) to validate programmatic results and the UNAIDS’ data model.
PEPFAR conducted the first three PHIAs in Zimbabwe, Malawi, and Zambia. The surveys validated the expanded data on the age and sex of clients that PEPFAR had been collecting from individual sites. In addition, the figures on HIV incidence and prevalence generated by the surveys closely tracked with the estimates produced by UNAIDS.
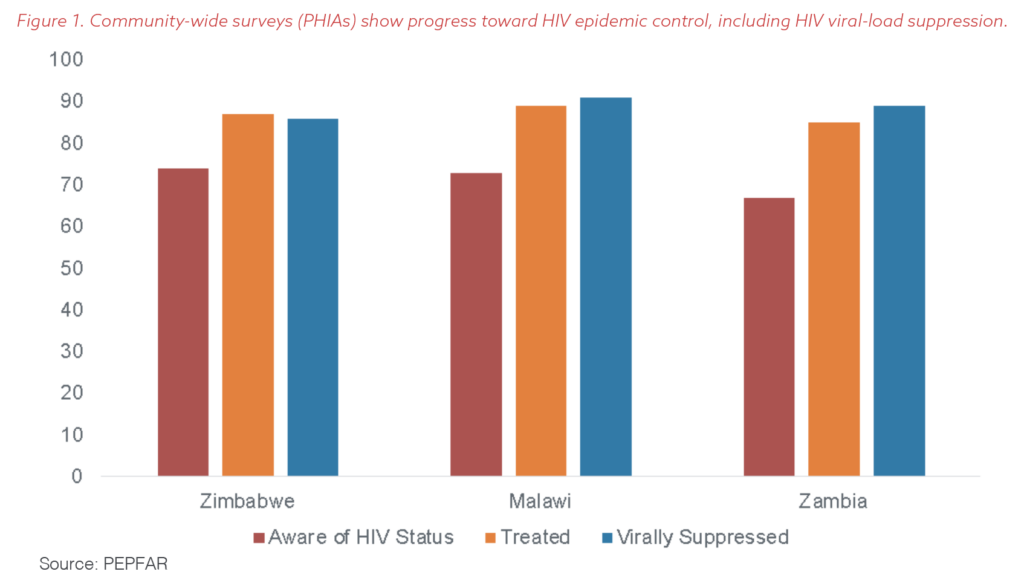
The PHIA data also showed that PEPFAR’s 2014 and 2015 realignment of services and funding based on need was working: The program was reaching and testing more individuals and putting more clients on lifesaving ARVs while ensuring they were staying on their medication consistently so there was no evidence of virus circulating in their bodies (called being virally suppressed). Overall, as Figure 1 shows, nearly 70% of all adults across the three countries knew their HIV status, over 80% of those who were HIV-positive were on treatment, and nearly 90% of those on treatment were virally suppressed. More than anything, the PHIAs demonstrated the deep commitment by clients to get treatment and stay on it.
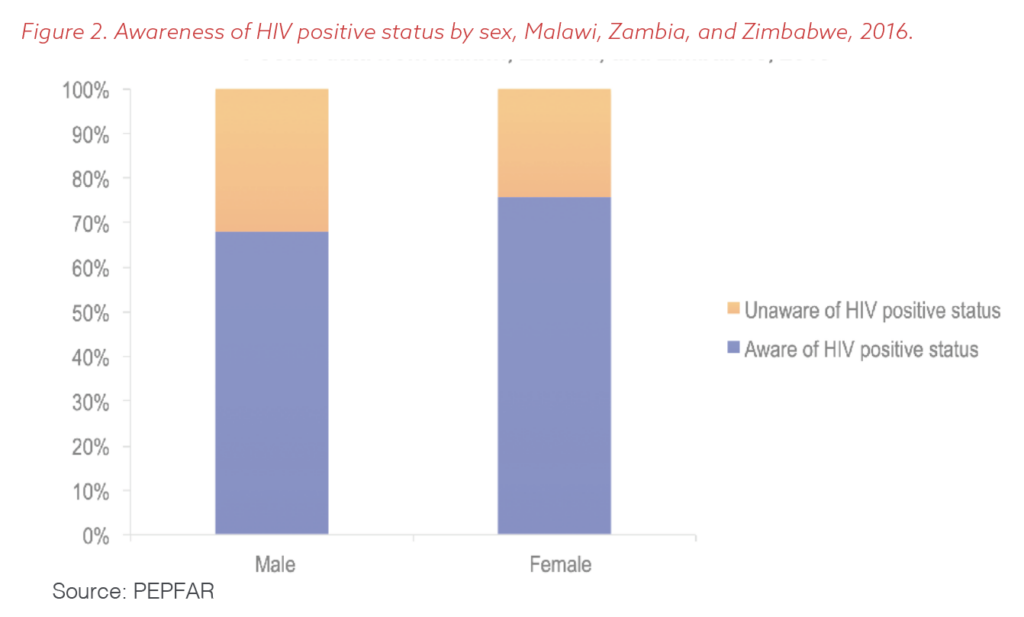
 But clear warning signs still existed, despite this great progress. The PHIAs offered unmistakable evidence that PEPFAR’s programming was not reaching some clients, and they identified the missing groups by sex, age, and geography. In particular, men of all ages were less likely to know their status and seek access to treatment than women, as shown in Figure 2.
But clear warning signs still existed, despite this great progress. The PHIAs offered unmistakable evidence that PEPFAR’s programming was not reaching some clients, and they identified the missing groups by sex, age, and geography. In particular, men of all ages were less likely to know their status and seek access to treatment than women, as shown in Figure 2.
This made sense, as routine primary health care at the community level in sub-Saharan Africa has historically targeted pregnant women, not men. Men simply were not seeking out care in large numbers until they were very sick; they were appearing in hospitals very late in their disease course, often with severe immunodeficiency and tuberculosis, when the ravages of HIV had done such profound damage that their lives would be shortened.
In addition to missing men, fewer than 50% of young adults, regardless of gender, knew their status. They therefore were less likely to access treatment and be virally suppressed, as shown in Figure 3.
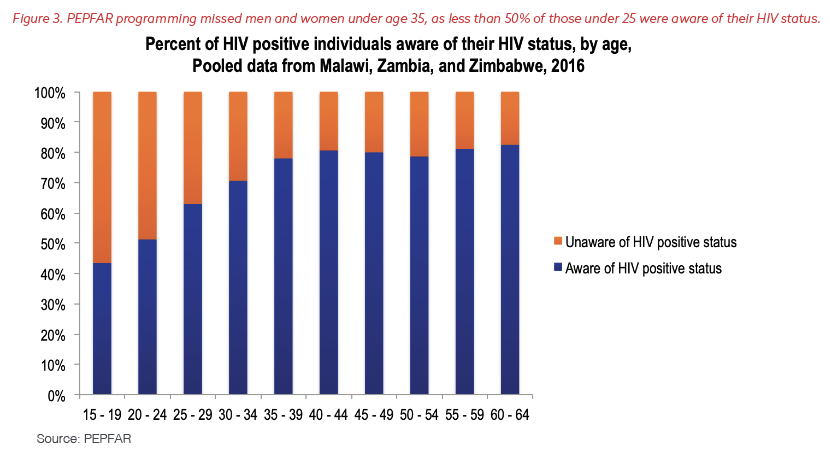
The PHIAs provided an independent evaluation of progress toward controlling HIV, but also a much more focused picture of the critical need to prevent new HIV infections among those at the greatest risk. After analyzing the PHIAs and triangulating the data with national census information, the Office of the Global AIDS Coordinator, PEPFAR’s partners, and national governments knew how big a problem they had on their hands in meeting the 95-95-95 targets and the global goal to end AIDS. Host governments and partners in every country needed to innovate to address the barriers to health care for men of all ages and to develop new programming and outreach to young men and women and other vulnerable groups.
But knowing who PEPFAR’s programming was missing was only the first step. The second was closing the gaps and addressing the barriers to health care for men and young people from the ground up in every country and county. In partnership with communities, PEPFAR needed to be able to reach early-stage HIV patients, the ones who had recently acquired the infection, felt healthy, and did not see the need to seek care.
“[PEPFAR] recognizes that social inequalities between women and men, in conjunction with harmful gender-based cultural norms and practices, not only perpetuate women’s vulnerability to HIV but also continue to fuel the HIV epidemic among both men and women.”
– PEPFAR annual report to Congress, 2005
Unique risk of HIV for adolescent girls and young women
President George W. Bush and Mrs. Laura Bush insisted that women be at the center of PEPFAR’s design and implementation. The fact sheet issued when PEPFAR was created in 2003 described how the program’s original model was based on the $500 million Mother-and-Child HIV Prevention Initiative announced by the president the year before. PEPFAR also set an expectation that every service-delivery site should count male and female clients separately. As a result, women were the majority of the beneficiaries of PEPFAR’s interventions in its early years: Women made up almost 60% of the people who received treatment through PEPFAR and 69% of those who underwent testing and counseling for HIV, according to PEPFAR’s first annual report to Congress, issued in 2005. The report promised a “continued emphasis on improving prevention services for vulnerable girls and young women,” and more women than men received treatment, care, and prevention interventions during PEPFAR’s first years.
On the ground, PEPFAR translated this call to action into scores of coordinated initiatives to reduce stigma, address harmful male norms and behaviors, reduce violence and coercion against women, improve girls’ and women’s access to income, and increase women’s legal protection. In South Africa, PEPFAR funded Men as Partners to collaborate with traditional leaders, trade unions, local nongovernmental groups and others to change high-risk cultural norms and increase men’s sense of responsibility for preventing the transmission of HIV. In Kenya, PEPFAR assisted the National Commission for Human Rights in working with community elders to change traditions that had restricted women’s ability to inherit property. Many PEPFAR-supported treatment clinics and care sites added income-generating activities for female clients and PEPFAR-sponsored savings clubs for women throughout sub-Saharan Africa. Initiatives led by local advocacy organizations with financial and diplomatic support from PEPFAR pushed to toughen laws against violence aimed at women and children and to change public perceptions.
Nevertheless, deeper dives into the data produced by the PHIAs showed the stark reality that women and girls between the ages of 15 and 29 were significantly more likely to acquire HIV than boys and men in the same age range. In some countries, the risk of HIV acquisition after age 15 was between five and 14 times greater in young women than young men and increased year after year into adulthood, as demonstrated by Figure 4. This trend contrasted with uniform and low rates of HIV infection among male and female children under 15 after years of progress in preventing the transmission of HIV from mothers to their children.
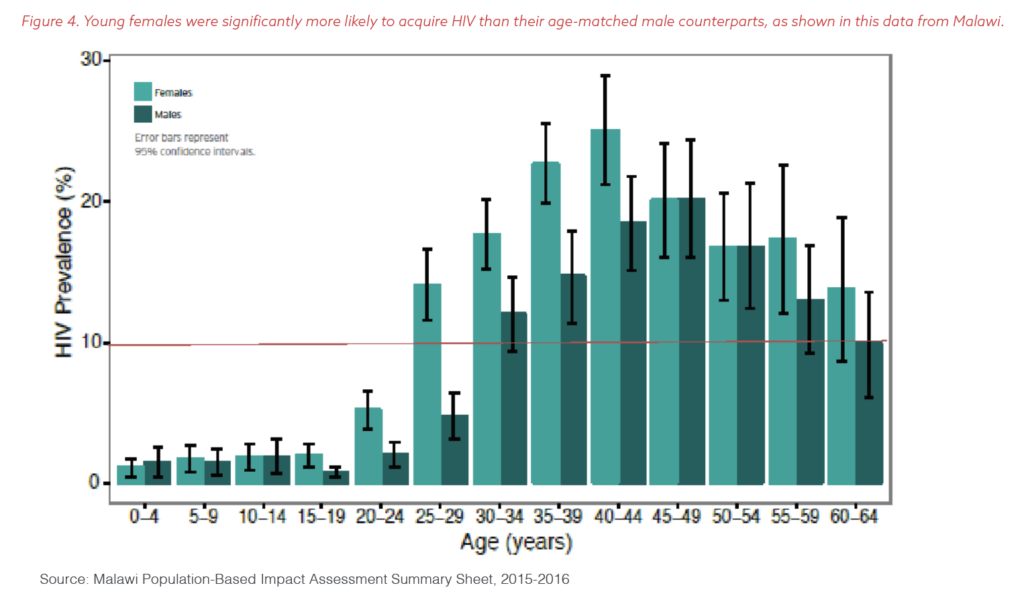
Global census data at the same time showed the population of young people in sub-Saharan Africa was surging, with 30% more young women than at the beginning of the pandemic, as illustrated by Figure 5.
DREAMS: PEPFAR Pivots to Invest Even More in Young Women
“If the world is to succeed in the effort to defeat HIV/AIDS, the soaring infection rates among women and girls simply must be reversed….”
– PEPFAR annual report to Congress, 2006
Once the data pointed to the threat to girls and young women, PEPFAR realized it needed to get into communities and listen to young women to understand the cultural, social, and institutional challenges that were putting them at an increased risk of acquiring HIV. Then, in deep partnership with local leaders and adolescent girls and young women themselves, PEPFAR’s implementing partners worked together to design programming focused on meeting the unique needs of this population. Funding was only part of the solution; new policies and culture change were key.
PEPFAR collected science and data on what interventions would have an impact, based on credible studies, as Figure 6 shows. PEPFAR then launched a comprehensive program called “DREAMS,” for Determined, Resilient, Empowered, AIDS-Free, Mentored, and Safe. Each word recognizes the need to address the full spectrum of risk and unique vulnerability of young women. The vision included making sure adolescent girls and young women could enroll and stay in secondary school and providing bridges to employment. Figure 7 illustrates the core package of interventions under DREAMS.

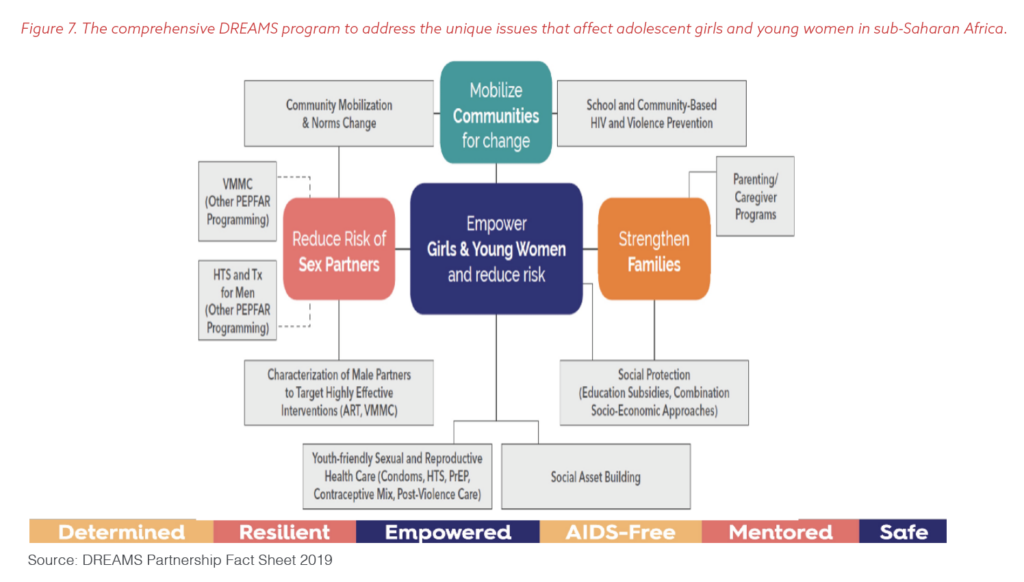
At the same time, the program set up clear metrics to track real-time progress in improving and achieving outcomes. PEPFAR worked with community leaders and governments to develop new policies to increase access to prevention services and remove more structural barriers for adolescent girls and young women. Ensuring action and the implementation of the new policies, such as working with local chiefs to decrease child marriage in their communities, was critical to the process.
Combating Child Marriage

PEPFAR also worked with its partners, families, and communities to ensure girls were protected during their travels to and from school, that bathrooms and dormitories were safe, and young women had access to medical care and knowledge.
The DREAMS program for adolescent girls and young women was set up as a public-private partnership. The private sector brought insights into age-segmented “marketing” and the importance of language- and age-specific media and social-media platforms. DREAMS took a client-centered approach, which tailored programming to specific age groups and focused interventions based on the unique risks and needs of each.
PEPFAR also developed the DREAMS Ambassador program, which was key to the development of peer role models and persistent advocacy. Young women became passionate champions for the support they needed to ensure they could thrive and were essential in driving further policy changes to prevent sexual violence and increase access to schooling. After only a year, the DREAMS Ambassadors were sharing the stage at events with their national ministers of health, raising the core issues that increased their vulnerability to HIV and gender-based violence and decrying the stigma and discrimination that were pervasive in health care. Adolescents told the hard truth that they felt they could not come to clinics to get knowledge about their own sexual health without facing discrimination and gossip from staff and other clients.
These frank conversations between the young women and their ministers drove awareness and policy change. In 2014, the African Union launched a “Campaign to End Child Marriage” and, by 2020, 13 African parliaments had set the age of marriage consent to 18, according to data from Girls Not Brides. The DREAMS Ambassadors were also peer community leaders and provided outreach to additional vulnerable adolescents and young women. The young women showed their communities that, with a small investment, they would lead. This created a ray of hope for all young women that a different future was possible.
Two elements were critical to the success of the program: First, continuous feedback from beneficiaries on what was working and not working and what needed to be strengthened or stopped. Second, quantitative data, including on who was and who was not accessing the DREAMS programming, the degree of engagement of participants in the modules, and the program’s outcomes and impact. PEPFAR’s partners carefully collected data in the districts in which DREAMS operated and compared them to the numbers from others. In parallel, PEPFAR conducted repeat community surveys.
In 2020, PEPFAR’s staff compared that year’s data with those from 2015. Across the board, the data showed a significant decline in HIV infections in young women, both between the ages of 20 and 24 and between the ages of 25 and 29. Panels A and B of Figure 8 show the specific results from Malawi and Uganda, respectively. The surveys demonstrated that well-designed and implemented collective programming on the ground, including DREAMS, could have a real impact in the highest-risk communities.
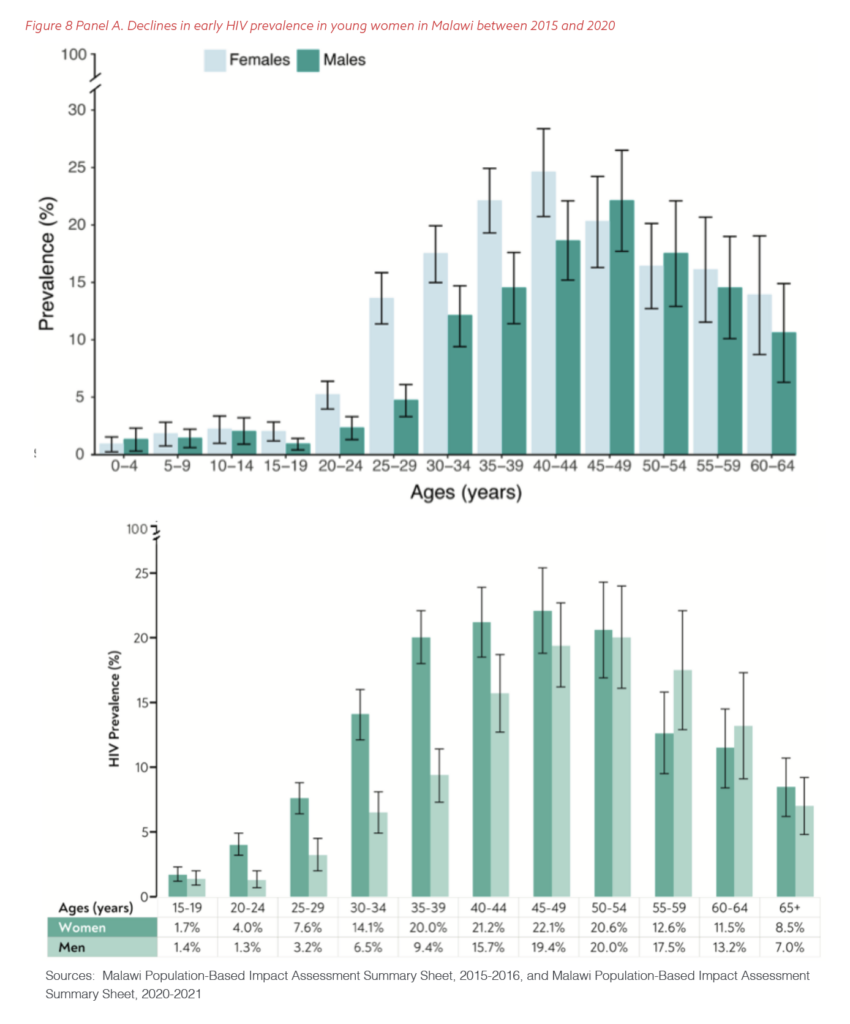
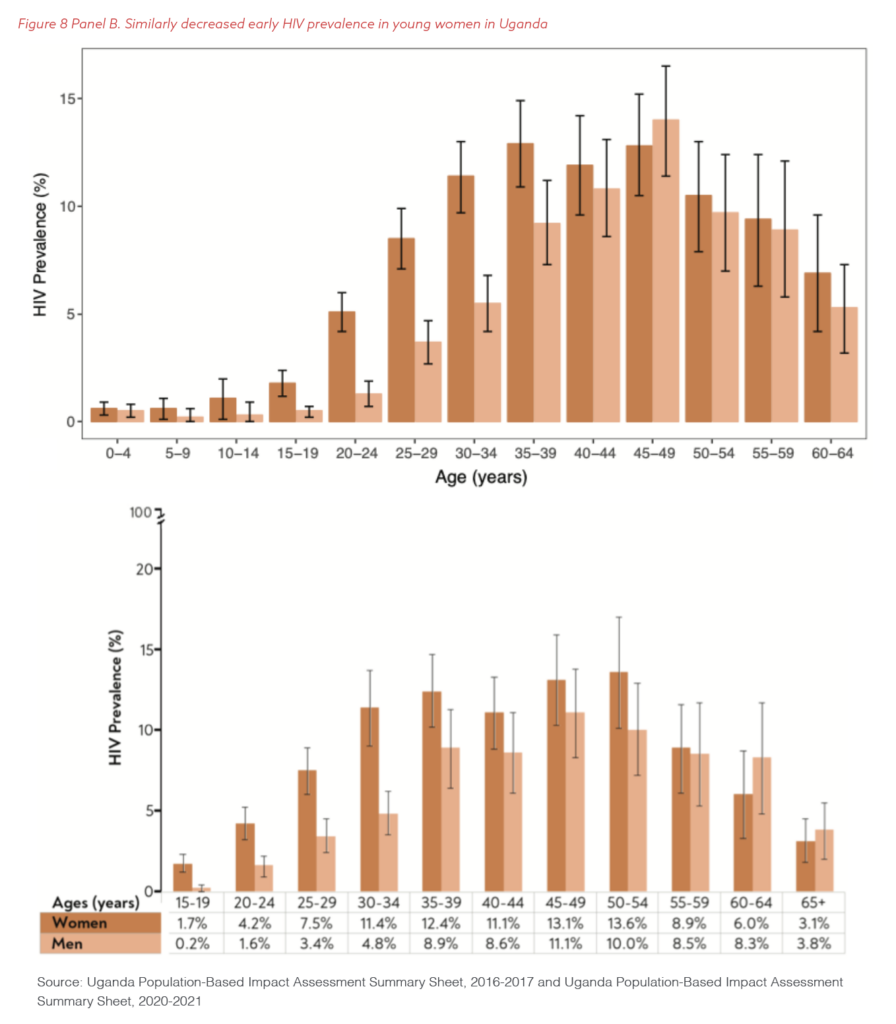
The client-centered approach became the standard of practice as PEPFAR continued to expand and fund its relationship with women and girls most affected by HIV through local partners, community leaders, and organizations. PEPFAR invested over $1 billion in DREAMS programming over the first five years of implementation out of a total bilateral investment of $20 billion during that time.
Pink Ribbon Red Ribbon and Go Further: PEPFAR Intervenes to Save Women’s Lives a Second Time
A new threat to women’s lives emerged at the same time PEPFAR was increasing its investment in young women to cut their rates of HIV acquisition. During one of President and Mrs. Bush’s trips to Africa after leaving office, some local women expressed gratitude for the lifesaving ARVs brought by PEPFAR but noted that many other women were now dying from something else: an aggressive form of cervical cancer. The issue had only become visible once women increasingly began surviving HIV and living longer lives.
President and Mrs. Bush were alarmed and wanted to act to change the future for these mothers and grandmothers, as they did with their original vision for PEPFAR, this time by preventing deaths from cervical cancer. They learned that women who are HIV-positive are up to six times more likely to develop invasive cervical cancer. But cost-effective solutions for early detection and treatment were available, PEPFAR’s local teams and leading authorities in obstetrics and gynecology in sub-Saharan Africa told them.
In 2010, President and Mrs. Bush and the Bush Institute launched Pink Ribbon Red Ribbon (PRRR), an innovative partnership to leverage public and private investments in global health to combat cervical cancer and breast cancer, the two leading causes of cancer death in women in sub-Saharan Africa and Latin America. It received funding and technical support from PEPFAR, thanks to a collaboration with Secretary of State Hillary Clinton. Led by the Bush Institute, PEPFAR, Susan G. Komen for the Cure, and UNAIDS, the PRRR partnership joined with foundations and companies to expanded the availability of vital screening and treatment for cervical precancerous lesions – especially for high-risk HIV-positive women – and also promoted breast cancer education and clinical breast examinations. As the stigma around cancer remains high, especially female cancers, PRRR also worked at the community level to promote cancer awareness; ensure communities understood that diagnosis and treatment were available; and expand the delivery of vaccines against the human papillomavirus (HPV), which causes cervical cancer.
Focusing in a small number of countries with high rates of cervical cancer, PRRR laid important groundwork to scale up programs to prevent, screen for, and treat cervical cancer and vaccinate adolescent girls against HPV. It supported ministries of health in establishing policy frameworks for national cancer control programs; collaborated with locally based providers to develop context-appropriate clinical guidance and standard procedures; raised the discourse around cervical cancer globally, especially among first ladies, African governments, and funders; and helped develop a global toolkit to facilitate the use of data in cervical cancer programs.
Five years on, however, the program was not screening as many women for cervical cancer, especially those living with HIV, as the Bush Institute had hoped. So the Bush Institute, in partnership with PEPFAR and UNAIDS, led a deep dive into PRRR to look for lessons that might shape a new approach to increase outcomes and impact. Based on recommendations from active listening, including through sessions in communities and with local organizations, the partners involved in PRRR realigned their focus, funding, and human resources to launch Go Further in May 2018.
“Over the past year, the Bush Institute has worked with Ambassador Deb Birx and PEPFAR on a bold new strategy. And, this week we are announcing the next phase of our partnership with PEPFAR and UNAIDS: a plan to effectively eliminate cervical cancer amongst HIV-positive women within a generation.”
— President George W. Bush, May 10, 2018, announcing the launch of Go Further
Go Further is a cutting-edge public-private partnership among PEPFAR, the Bush Institute, UNAIDS, Merck, and Roche aimed at ending AIDS and cervical cancer in sub-Saharan Africa within a generation. The partnership’s goal is reducing new cervical cancer cases by 95% among the estimated 11 million women who are living with HIV in 12 African countries which have some of the highest rates of HIV and cervical cancer in the world. Go Further invests directly into communities and local partnerships that are integrating and scaling up screening and treatment services for cervical cancer within existing platforms for HIV treatment and women’s health.
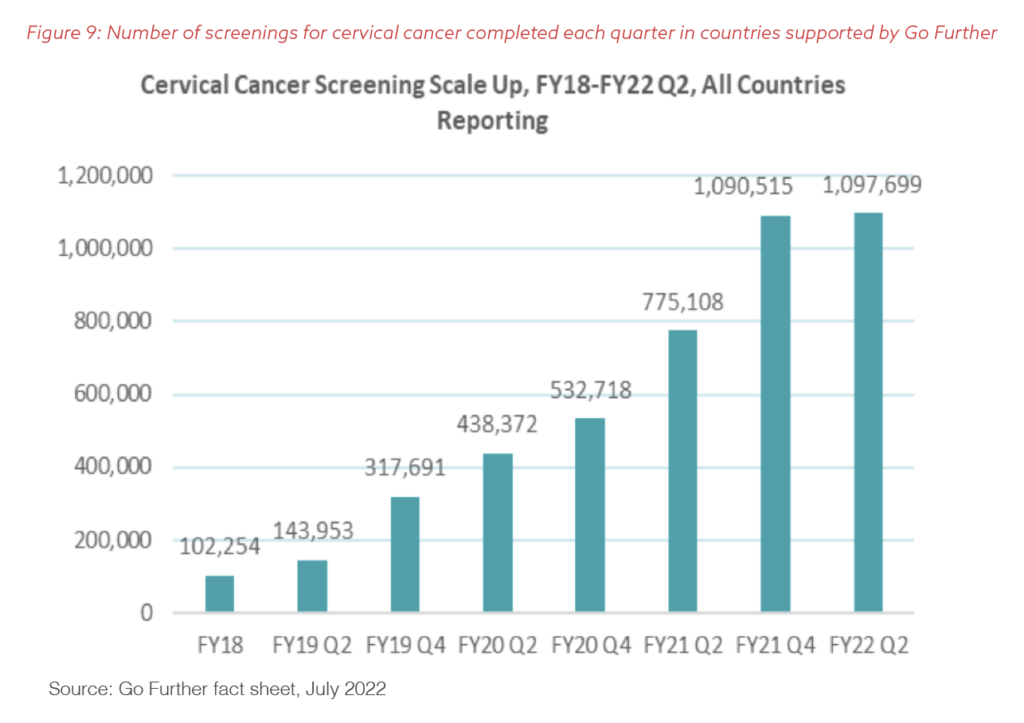
Shifting the implementation, monitoring, and evaluation of the program to PEPFAR resulted in impressive and rapid scale-up. From 2018 to 2021, PEPFAR, as part of Go Further, has supported nearly 4.5 million screenings for women who are living with HIV, nearly nine times the number of screenings PRRR was able to achieve in five years for all women, as illustrated in Figure 9. Through Go Further, 33 times as many women living with HIV have had access to a cervical cancer screening for the first time in their lives.
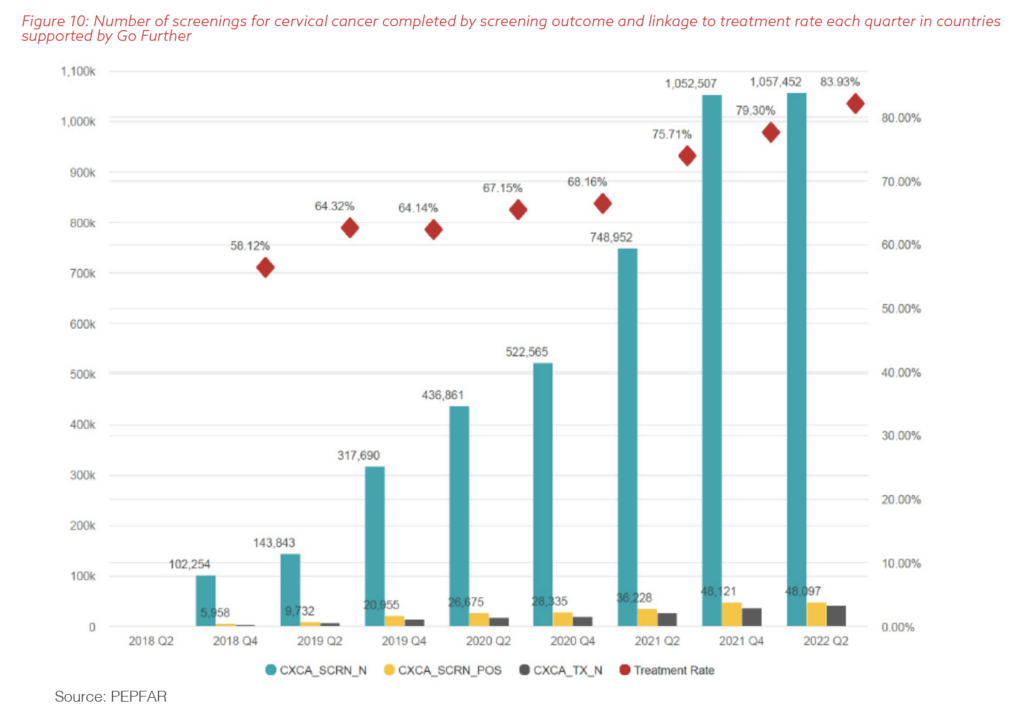
Continually evaluating the program and speaking with providers, implementers, and clients, Go Further’s partners identified early gaps in linkage to treatment. Using this feedback, Go Further also has steadily improved the number of women who are able to access necessary treatment for precancerous cervical lesions each quarter, as shown in Figure 10.
PEPFAR’s unrelenting focus on data and the partners’ decision to hold each other accountable and leverage each one’s unique strengths made this evolution of programming possible. The very founding principles of PEPFAR as a data-driven, transparent program allow Go Further to achieve continuous quality and programmatic improvement.
The results shown in Figures 9 and 10 were made possible by the thousands of mothers, sisters, and daughters who bravely confront HIV and cervical cancer diagnoses every day.
PEPFAR Changes Its Models to Reach Men on Their Terms
PEPFAR also had to change its approach to reach some of the men it was missing. Even after 10 years of programmatic implementation, young men were not accessing testing and treatment, and men of all ages were showing up in clinics and hospitals with late-stage HIV, many co-infected with tuberculosis, often too late to save their lives. To understand the problem, illustrated by PHIA data and information from PEPFAR sites, PEPFAR and the private sector held focus groups with men to delineate their barriers to access.
With data as the starting point, PEPFAR and its partners worked together to develop new programming and made continuous improvements to address the gaps and challenges men had described, community by community and age band by age band. Local groups across PEPFAR innovated to create unique primary care opportunities for men, such as opening clinics early in the morning and keeping them open later in the evenings so men could stop by on the way to and from work. In another example, Lesotho created male spaces in clinics so men could be seen by male nurses and physicians.
Building on the successful models of DREAMS and Go Further that served women, PEPFAR formed a new public-private partnership around men’s health in mid-2018: MenStar Coalition. It included PEPFAR; the Elton John AIDS Foundation; Unitaid; the Global Fund to Fight AIDS, Tuberculosis and Malaria; the Children’s Investment Fund Foundation; Johnson & Johnson; and Gilead Sciences. MenStar supported innovative approaches to delivering effective HIV/AIDS services for men to increase their rapid uptake of HIV testing, improve linkages to HIV treatment, and support the individual achievement of viral suppression. MenStar had defined goals of reaching an additional 1 million men with HIV treatment and achieving viral suppression in over 90% of HIV-positive men between the ages of 24 and 35 to interrupt HIV transmission to their sexual partners.
MenStar has made progress through multiple approaches: data analytics and human-centered design to adapt services better to men; nuanced messaging to persuade men to seek care; and targeted consumer marketing. Innovations such as HIV self-testing and supply-side solutions, including male friendly strategies for HIV service delivery – such as dedicated men’s corners at existing health clinics, expanded clinic hours, pickup points outside clinics for stable patients, and multimonth prescriptions – were also critical, as was ensuring essential HIV commodities and services were available to meet increased consumer demand. This community-grounded, client-centered, data-driven program has been highly successful, achieving the goal of an additional 1 million men on treatment within 24 months.
Reforms promoted by PEPFAR and instituted by national and provincial governments, which have devolved responsibility for much of the health care in many countries, have promoted flexible, safe, and sustainable access to ARVs. These changes included creating men’s treatment clubs; permitting health workers to dispense three or six months of medications (instead of monthly packages, which had required clients to make an often-expensive and time-consuming trip to crowded hospitals and clinics every 30 days); and switching to a better-tolerated drug, DTG. These advancements not only improved access for young men, young women, and men across all ages, but became the solution to serving all clients during the COVID-19 pandemic, when travel was limited and access to health care constrained.
PEPFAR Confronts Stigma to Save the Lives of Marginalized People
These lessons learned from peer-led outreach and community-led implementation, along with the continuous use of data, are the hallmarks of PEPFAR’s successful partnerships. But the achievements of these programs in such a short period of time also laid bare the lack of progress among the most vulnerable and marginalized clients.
From the beginning, PEPFAR understood that additional marginalized populations beyond young women continued to be at higher risk and that policy changes were needed to ensure access to critical interventions. The most at-risk, yet most poorly defined, “key populations,” include people who inject drugs (PWID), men who have sex with men (MSM), prisoners, sex workers, and transgender persons. In 2004, PEPFAR added Vietnam as its 15th “focus country” to respond to the growing epidemic of HIV among key populations there and introduced targeted interventions in other countries with “concentrated” epidemics, such as Guyana.
In all the focus countries, PEPFAR pursued a comprehensive strategy for prevention and treatment among key populations, which included a number of elements outlined in PEPFAR’s annual report to Congress in 2005:
- Building on existing community organizations and social networks to expand counseling, mentoring, and peer outreach.
- Delivering interventions to prevent and treat substance abuse among HIV-positive individuals, including for those who inject intravenous drugs.
- Promoting a comprehensive package for sex workers and other high-risk groups, including offering counseling and testing for HIV at mobile and fixed sites, screening for and treating other sexually transmitted infections, and promoting the correct and consistent use of condoms.
- Designing and carrying out media interventions with specially tailored messages appropriately targeted to specific key populations.
- Combating the sexual coercion and exploitation of young people and women.
In the program’s first year alone, PEPFAR funded more than 500 community-outreach programs aimed at key populations, which reached almost 12 million people, according to the annual report to Congress. Examples include Corridors of Hope in Zambia and the Lakay Social Clubs and “Other Choice” initiative in Haiti, all of which provided prevention information and tools to sex workers, along with education and economic alternatives if they chose to leave sex work.
“Aggressive prevention strategies among people who engage in high-risk activity are critical to stop the spread of infection….”
– PEPFAR annual report to Congress, 2005
Because of the vulnerable nature, stigma, and punitive policy environments faced by many of these key populations, it was difficult to estimate their sizes, and host-country leadership often undercounted them for political or ideological reasons. This sometimes led to the mistaken conclusion that all gay and bisexual men, sex workers, and transgender persons had been reached with prevention and treatment interventions. However, through quiet community diligence, peer-outreach workers calculated the size of this population was 10 to 100 times larger than governments’ numbers and differentiated it by community and geography.
These fundamental differences in size estimates generated by communities, partners, and the host governments, combined with the punitive legal and sociocultural environment facing key populations in many countries, made community outreach, prevention interventions, access to treatment and clinical care unnecessarily challenging.
Nevertheless, PEPFAR’s partners on the ground have worked tirelessly to provide peer outreach and safe spaces for education, prevention, and treatment services. Policies and policy reforms to ensure access to lifesaving prevention and treatment services are highly variable by country, by community, and by risk group. In many countries, services are more available for PWID or sex workers than MSM. In other countries, the situation is the opposite. High levels of stigma and discrimination and fear of reprisal continue to drive vulnerable people into the shadows and out of care or become barriers to any care.
For this reason, discretion and trust are critical, and services for key populations must be available, including through nongovernmental partners, with minimal data sharing with host governments. This is an area that still needs criminal and policy reforms and better programmatic implementation and access to ensure no one is left behind. Some of the same strategies that have worked with adult men in general in countries like Zambia also have proven successful with key populations: treatment clubs, multimonth dispensing of medications, and substituting DTG for older drugs that caused more side effects. The elimination of formal and informal fees for services in public-sector health facilities has removed a major disincentive for members of marginalized groups to seek care and begin and stay on treatment.
The paucity of data, the lack of concurrence on the numbers, and the dearth of policy reforms needed to improve access to prevention and treatment services for key populations will continue to drive HIV risk into the shadows and keep programs from achieving the 95-95-95 targets and the goal of ending AIDS by 2030. Around the globe, the countries or regions with an HIV epidemic primarily concentrated in key populations, whether in Russia, Indonesia, North Africa, or Central America, lag behind others in expanding treatment coverage for ARVs, decreasing AIDS fatalities, and reducing HIV prevalence. This worldwide trend is best illustrated by the dramatic differences between new HIV infections in Ukraine and Russia, as shown in Figure 11.
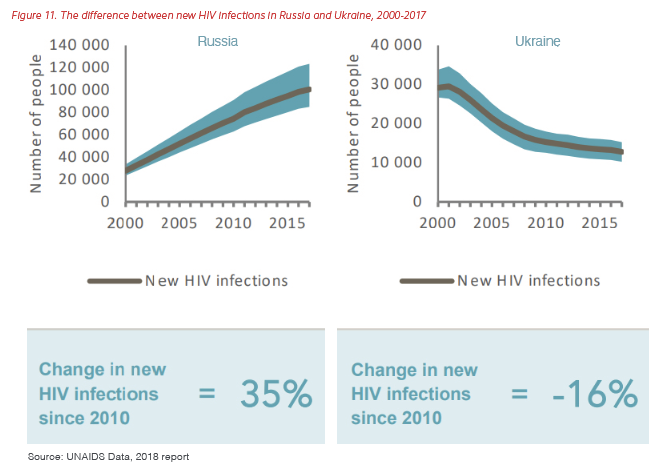
In Ukraine, all levels of public-sector leadership, from mayors to the president, committed to addressing the HIV epidemic in the country independent of risk factors. Three elements were critical to their response. The first was developing an enabling environment that encouraged access to prevention and treatment services for marginalized populations, including PWID and MSM. The second was direct funding of peer and nongovernmental programs by the public sector, including by altering policies to ensure the funding of programs led and trusted by the communities at risk. Finally, the national government financed evidence-based prevention and treatments for marginalized populations, including medically assisted treatment (MAT) for PWID; condoms, lubricant, and preexposure ARV treatment (PrEP) for MSM; and trusted access points for the delivery of both HIV prevention and treatment services.
On the other hand, Russia’s number of new infections has increased because the government has continued with a legal framework that drives vulnerable populations further from services and does not recognize interventions known to prevent new infections, including MAT.
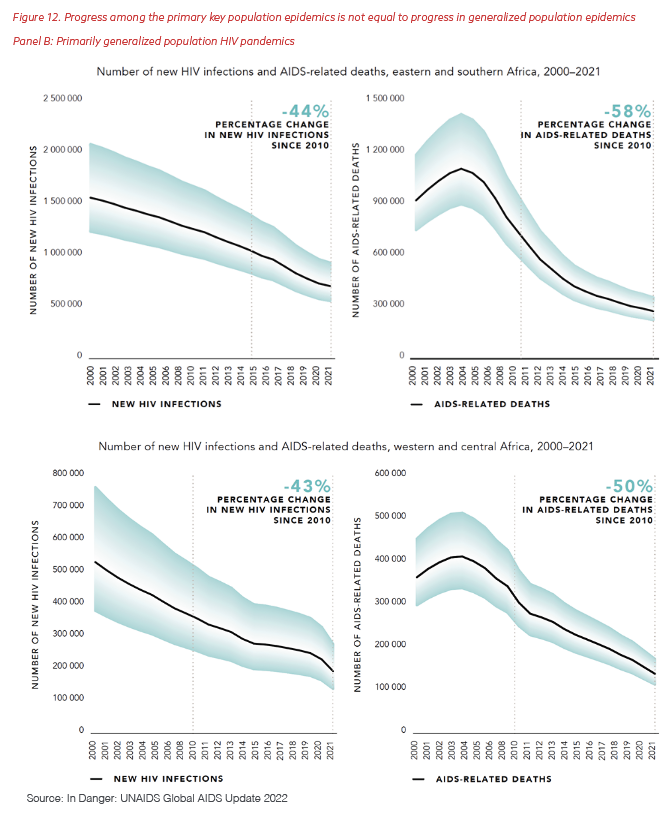
The problem is not just funding: Political will is needed to change policies and implement programs in new ways. Policies must keep pace with epidemics as they move through populations and evolve to ensure equity among all communities. Gaps in access to prevention and treatment programs must be continually addressed in partnership with communities and governments. Going forward, the lack of progress in controlling epidemics concentrated in key populations, as shown in Panels A and B of Figure 12, needs urgent attention from PEPFAR, other funders, and national governments. Countries with epidemics primarily among key populations (Panel A) lag dramatically behind the progress seen in countries with generalized epidemics (Panel B), both in decreasing new infections and preventing deaths. In addition, the epidemics among key populations that persist within the generalized pandemic of HIV in sub-Saharan Africa also require solutions for these countries to meet the global goal of ending AIDS.
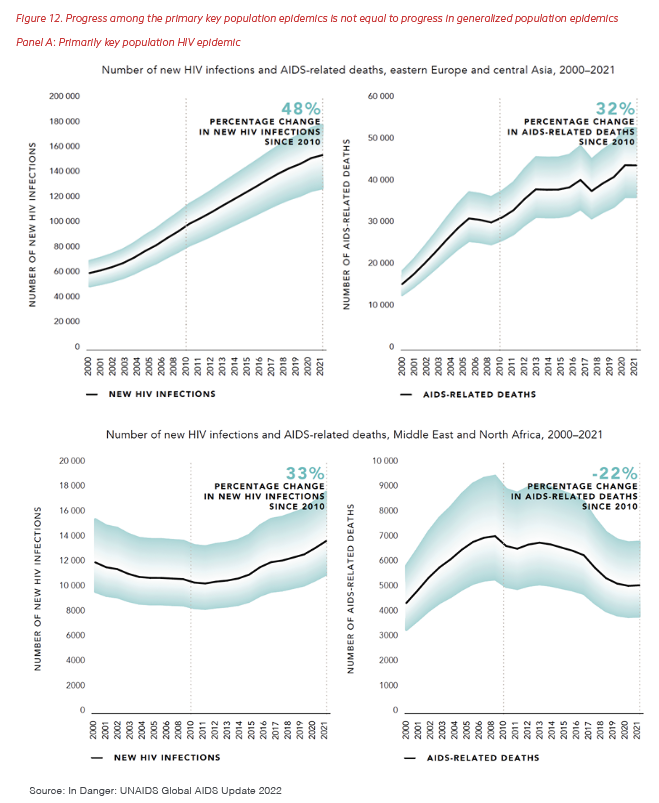
Every successful program within PEPFAR started with the identification of the population not being served, deep and consistent communication with the communities at risk, programming specifically focused on addressing the structural barriers and access to care, and continuous program evolution based on the changing needs of the community. As the program begins its third decade, PEPFAR must take this same approach to the concentrated HIV epidemics among key populations in all the countries in which it works, including by promoting policy reforms, supporting peer outreach, and directly funding peer-led services offered by local organizations.
Summary
Policies and practices to combat HIV/AIDS work best when coupled with detailed data to drive programmatic decisions and future direction. Money alone is never enough to guarantee programmatic success. Ensuring a program meets its goals requires the constant use of data, always evaluating who is being reached and who is missing. It necessitates innovation informed by the experience of individuals closest to, or from, the community and the creation and maintenance of political will and a policy environment that allows interventions to reach communities most in need. Most important is accountability for prioritizing and investing in the right areas to make the right impact.
Together, as a world community, we need to address the large gaps in access to HIV prevention and treatment among key populations around the globe. Twenty years into PEPFAR, the persistent shortfalls in programs for key populations demand a new model and a course correction with significant expansion and direct funding of peer-led local services outside the public sector. Policymakers and program leaders need to continue to integrate and analyze information from service-delivery sites with data from independent community surveys and evolve their interventions to remove persistent, structural barriers to access for both prevention and treatment services. In many clinics, the data are still only posted on the wall, so harnessing the numbers for decision-making will require electronic reporting and the appropriate training to make results available to communities and leaders. These steps will create a model for current and future success, not only for PEPFAR but for responses to any pandemic, no matter the pathogen that causes it.
Recommendations
The United States should learn from PEPFAR’s use of data and data analytics in the following ways to improve the U.S. government’s assistance overseas:
PEPFAR
- PEPFAR should look to the peer-service delivery model for both prevention and treatment services across the southern United States and Ukraine to inform how it addresses the HIV epidemic in sub-Saharan Africa, particularly in key populations.
- Building on the success of the Key Population Investment Fund, PEPFAR should prioritize expanding direct funding to local organizations and peer-led groups and ensuring their capacity to receive and manage the resources.
- PEPFAR should work to identify the at-risk communities still not being reached by its programming, including by increasing the PHIAs’ focus on specific key populations (with appropriate safeguards).
- PEPFAR should launch an independent community survey designed specifically for children by age bands to understand the poorly defined gap in access to lifesaving HIV treatment in that population.
- PEPFAR should articulate and translate the lessons of Go Further for integrated health care to serve people living with HIV across their lifespan.
PEPFAR and all U.S. government departments and agencies that implement foreign assistance for health and development
- Agencies should collect and analyze outcome and impact data in real time to ensure maximum impact for the dollars they invest.
- They should integrate programmatic data on the age, gender, race and ethnicity, and risk factors of their beneficiaries with information obtained through well-designed community-level surveys to identify gaps in coverage and address them immediately.
- They should analyze data down to the site level of implementation to learn from high-performing places that are innovating and provide those lessons across programs in a systematic manner.
- They should bring transparency to their funding and data by investing in partnerships with local nongovernmental organizations and community groups that enhance mutual accountability, exchange information in real time, and set and strive to meet measurable outcomes.
Congress
- Congress should encourage U.S. foreign assistance initiatives to pursue budgetary efficiencies to expand and improve their collection, reporting, and use of data to drive continuous programmatic improvement. This should offset any need for additional resources. But expanded data reporting can involve training, new or updated systems, and additional staff time and could necessitate additional resources.
Acknowledgements
The Bush Institute would like to thank Dr. Mark Dybul, former Executive Director of The Global Fund (2013-2017) and former U.S. Global AIDS Coordinator (2006-2009), and Dr. Jen Kates, Senior Vice President and Director of Global Health & HIV Policy at Kaiser Family Foundation, for their insightful feedback on and review of this paper.