Go Further has used data to support innovative approaches to close the treatment gap and ensure that every woman who needs treatment receives it.
Go Further, a partnership between the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR), the George W. Bush Institute, UNAIDS, Merck, and Roche, aims to reduce new cervical cancer cases by 95% in women living with HIV in 12 countries across sub-Saharan Africa; these countries have some of the highest rates of HIV prevalence and cervical cancer incidence in the world. We have the tools to prevent cervical cancer through HPV vaccination or by detecting and removing precancerous lesions before they become cancerous.
Of the 2.3 million screenings PEPFAR has completed as part of Go Further, nearly 6% have found precancerous lesions. For women living with HIV, their ability to stay cancer-free hinges on having these lesions removed before they progress to invasive cervical cancer.
Three types of treatment are currently used to remove precancerous lesions: cryotherapy, thermal ablation, and loop electrosurgical excision procedure (LEEP). Cryotherapy and thermal ablation can be done the same day as screening by a nurse, providing women living with HIV with a one-stop visit for cervical cancer services. LEEP is an out-patient procedure used to remove larger lesions and is usually done by a higher-level clinical provider such as a medical officer or doctor. Because LEEP requires a higher level of care, women are usually scheduled for the procedure at a later date.
The Go Further partnership aims to treat all women living with HIV found to have precancerous lesions, and we are diligently working toward a 90% minimum treatment rate to align with global targets. This is ambitious, but the Go Further partnership is committed to identifying and addressing the key barriers to ensure it is achieved.
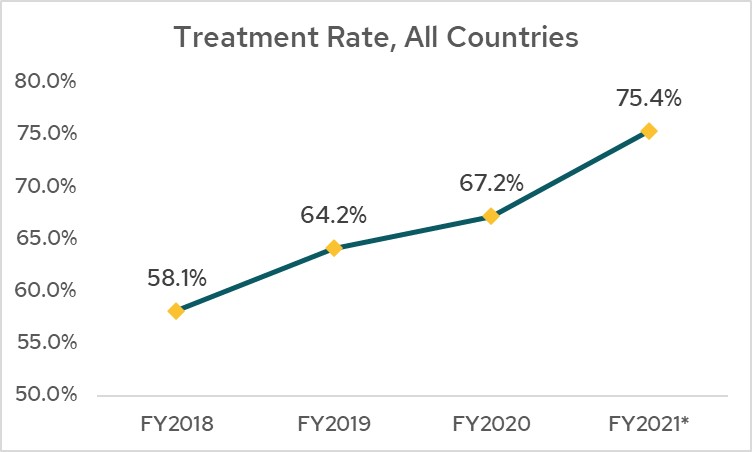
Go Further has increased cervical cancer treatment rates among women who have screened positive for precancerous lesions from 58% in fiscal year 2018 to over 75% at the midpoint of fiscal year 2021. But we still are short of our 90% target. There are a variety of factors that keep women from accessing same-day treatment services, including fear and stigma, the need to consult with partners about treatment and the required post-treatment abstinence period, and distance to and from a facility with appropriate treatment services.
The COVID-19 pandemic has compounded many of these issues. For instance, clients have been understandably hesitant to visit healthcare facilities for fear of contracting COVID-19. In some countries, cervical cancer services have been paused or scaled back with clinical staff redeployed to respond to the pandemic, leaving cervical cancer clinics and treatment centers short staffed. In addition, a rapid transition to six-month dispensing of antiretroviral (ART) drugs used for HIV treatment (a positive development) means that women living with HIV have not been accessing clinics as frequently as they had in the past.
Despite these challenges, Go Further has used data to support innovative approaches to close the treatment gap and ensure that every woman who needs treatment receives it. The PEPFAR teams, including the program staff, health care workers, and implementing partners, in collaboration with communities and ministries of health, are developing solutions to go further for women’s health. These strategies do not necessarily require new technologies, but simply different ways of using existing technologies or overcoming obstacles.
In Botswana, nurses carefully review the screening registries and dedicate time to call each client who did not receive a screening or treatment during their ART visit to ensure they are scheduled for an appointment. In the first six months of fiscal year 2020, Botswana had a treatment rate of 64%; in the first six months of fiscal year 2021, their treatment rate was as high as 86%. Thanks to the dedicated efforts of the nurses, doctors, and program staff, more women are getting the treatment they need for precancerous lesions.
Eswatini has increased the number of their screen-and-treat sites to reduce the distance clients must travel to access precancerous lesion treatment. They have also established partnerships between facilities to improve the availability of LEEP services, including providing transportation for clients who must travel long distances. These and other strategies led to Eswatini treating 98% of clients identified as needing it — the highest rate of all Go Further countries at the end of fiscal year 2020.
The team in Zimbabwe is working to scale their treatment efforts and there has been steady improvement. Innovative catch-up efforts like LEEP camps have helped reach women who need treatment and provided dedicated resources and staff to ensure that when women arrive for their treatment, they receive it. Despite the challenges presented by COVID-19, Zimbabwe saw its treatment rate grow from 49% to 57% in fiscal year 2020. By the midpoint of fiscal year 2021, their treatment rate was up to 65%.
Go Further will continue to work to achieve our goal of treating all women who need it, particularly by championing the solutions led by our partners in each country. Country teams and partners continuously innovate and find solutions to close treatment gaps. Each solution leads to more women receiving treatment for precancerous lesions, saving lives by preventing them from progressing to invasive cervical cancer. One woman lost to cervical cancer is one woman too many.




























